Upper GI Endoscopy
- Upper GI Endoscopy
- Colonoscopy
- ERCP
- Endoscopic Variceal Ligation
- Endoscopic Sclerotherapy
- Hemoclip Application
- Endoscopic Balloon Dilatation
- Fibroscan
- Biliary stenting
UPPER GI ENDOSCOPY IN NAGPUR
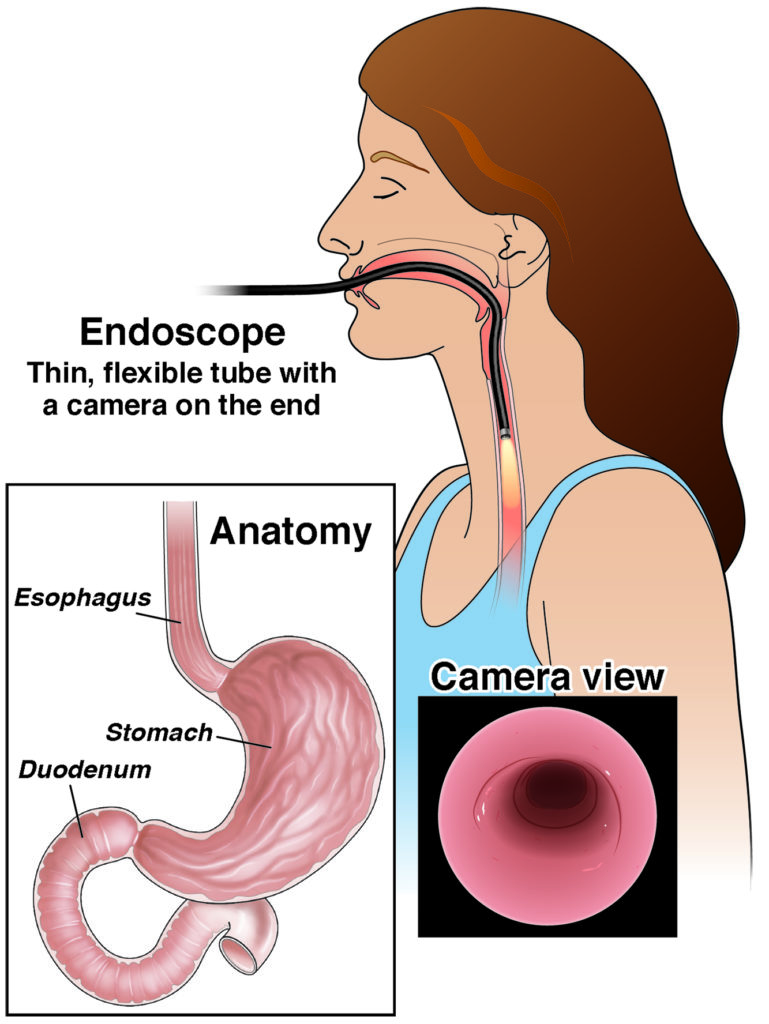
Upper GI endoscopy is a test which allows the doctor to look directly at the lining of the esophagus, stomach and duodenum. Diagnostic upper GI endoscopy is recommended for change in appetite, occult or frank blood in the stool, unexplained anaemia and as a diagnostic test for dyspepsia and reflux. In order to do the test, an endoscope is carefully passed through the mouth into the esophagus, stomach and duodenum. The endoscope is a long flexible tube, about the thickness of your index finger, with a bright light at its tip. The video camera on the endoscope transmits images of the inside of the upper GI tract to a monitor allowing the physician to examine the lining checking for any disease or abnormalities. If necessary, polyps or other types of abnormal tissue can be removed through the scope during upper GI endoscopy. Tissue samples (biopsies) can be taken during upper GI endoscopy as well.
Diagnosis
Upper GI endoscopy can help doctors diagnose the reasons for
Changes in appetite and early satiety
Pain in epigastrium and upper abdomen
Bleeding per vomitus or evaluation of unexplained bleeding from the gastrointestinal tract
Unexplained weight loss
To evaluate abnormalities in the upper GI tract in other imaging like ultrasound and CT scan
Unexplained anaemia
Nausea and vomiting of unknown cause
Diagnosis and surveillance of gastric ulcers and gastric cancer
Upper GI endoscopy can also detect inflamed tissue, ulcers (like in peptic ulcer disease or gastritis), and abnormal growths. The procedure is used to look for early signs of gastric cancer and GERD complications. The doctor can also take samples from abnormal-looking tissues during upper GI endoscopy. The procedure, called a biopsy, allows the doctor to later look at the tissue with a microscope for signs of disease.
Chromo-endoscopy: A dye is sprayed over gastric mucosa that will help to diagnose early tumours and helpful in gastric cancer surveillance especially in high-risk groups like patients with intestinal metaplasia.
NBI (Narrow Band Imaging): is a modality when applied with upper GI endoscopy can help to differentiate malignant lesions from benign gastric lesions without the need for biopsy or can help to direct biopsies from specific sites so that diagnostic yield is high.
Treatment
Upper GI endoscopy can help doctors with the following issues
Removal of gastric polyps (polypectomy)
Removal of large gastric polyps/tumours by endoscopic mucosal resection (EMR) or endoscopic submucosal dissection (ESD) which was earlier thought to be only removable by surgery
Dilate narrowed segments (stricture dilation) of the esophagus and place metallic stents across them (esophageal stenting)
Sclerotherapy for esophageal varices in liver disease patients
Control of bleeding from ulcers, vascular malformation, growth or a tumour
Removal of foreign bodies
Palliative treatment for obstructing tumour (metal stenting) or bleeding tumour (laser, electrocoagulation, heater probe, injection)
H. pylori eradication and assessment
Interventions
Polypectomy: polyps are removed by snare
Endoscopic Band Ligation (EBL) for varices: band applied for the prevention of variceal bleeding
CRE (Controlled Radial Expansion) balloon dilatation for stricture dilatation
Argon Plasma Coagulation (APC): bleeding vessels are coagulated
Endoscopic Mucosal Resection (EMR): polyps are removed by lifting them up by sub-mucosal injection
Endoscopic Sub-mucosal Dissection (ESD): tumours or polyps with deep extension are removed en-bloc or piecemeal with this procedure, surgery can be avoided.
SEMS (Self Expanding Metal Stent) placement: for obstructing cancerous growth that is not amenable to surgery, SEMS can be placed for symptomatic relief
Sclerotherapy/Glue injection for bleeding varices: in liver disease patients dilated veins (varices) which are bleeding can be obliterated by this technique
Preventive
Gastric cancer surveillance: gastric cancer is prevalent in Asian countries. Surveillance is recommended in high-risk patients like those with family history of gastric cancer, intestinal metaplasia, or chronic atrophic gastritis to detect this disease in the early stage which may help in endoscopic treatment avoiding surgery.
Surveillance of patients with GERD (Gastroesophageal Reflux Disease): Patients with long-standing GERD are prone to develop Barrett’s esophagus and esophageal cancer which can be screened by upper GI endoscopy combined with chromo-endoscopy or NBI.
Early detection and characterization of premalignant gastric lesions followed by removal: Early detection and removal of premalignant lesions prevents malignant transformation and future gastric cancer development.
H. pylori screening and eradication: Screening for H. pylori infection and appropriate eradication therapy prevents peptic ulcer disease and reduces gastric cancer risk in susceptible populations.
Book an Appointment
+91 8788982544
Locate us
Gondwana Square, Nagpur
siddiqui.amin10@gmail.com

